Thalassemia
Total Views |
What is Thalassemia?
Thalassemia is an inherited condition affecting the capacity of the body to produce blood. Thalassemia varies in severity requiring no treatment to severe forms requiring lifelong transfusions.
What is the cause of Thalassemia?
Oxygen in body is supplied by hemoglobin. Hemoglobin in adults has 4 chains 2 alphas and 2 betas. There are other types of hemoglobin which have a slightly different kind of chains; however they are not very severe usually. In Thalassemia, there are genetic mutations because of which the capacity of the patient to produce these chains is decreased. Thus many types of Thalassemia are possible according to the mutation and the chain affected.
What types of Thalassemia?
Clinically important types include
- Thalassemia trait. These individuals are asymptomatic, with hemoglobin hovering around 9-12. They don’t require any treatment, however it is important to recognize this condition so that genetic screening can be advised to expecting parents and transfer of the problem to next generation can be prevented.
- Thalassemia Intermedia: These patients have a slightly more severe type of Thalassemia. Hemoglobin is usually . They require transfusions in times of stresses like during surgeries, during pregnancy or during puberty and infections
- Thalassemia Major: These children usually present in young age, usually before 2 years of age with low hemoglobin. If not noticed early these kids can have recurrent infections, distended abdomen, stunted growth. If not recognized in time these kids can die of shortage of blood. Once diagnosed these patients will require transfusions for life.
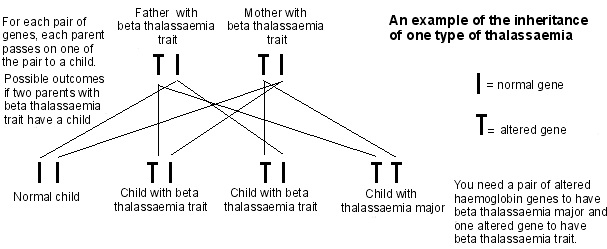
How is Thalassemia Inherited?
If the genetic mutation is inherited from both parents, it usually severe type of Thalassemia otherwise it is Thalassemia trait.
What is the treatment of Thalassemia major?
It includes lifelong blood transfusion at a monthly to monthly interval with the aim of keeping hemoglobin >9 gm%. With chronic transfusions, these patients can develop iron overload and as a result these patient can have various organ dysfunction from the excess iron deposits in various organs. Majorly the organs affected included the heart, liver, reproductive organs being a few of them. These patients are as a result treated with lifelong chelation with the aim of decreasing the iron overload and thus preserving the liver, heart of the patients.
These patients thus have to depend on lifelong transfusions and chelation. Also they will require lifelong investigations for monitoring the effects of chelations.
Is there a cure for Thalassemia?
Yes. The patients of Thalassemia major can undergo bone marrow stem cell transplant and be cured from Thalassemia. These patients after a successful transplant will never require transfusions.
What is the success of Bone Marrow transplant?
Success of transplant depends on a lot of things. In a nicely planned transplant, success rates are as high as 90%. Earlier the transplant and with a matched sibling transplant the chances of good results are maximum, so it is advisable to contact your transplant physician as soon as possible.
Is it possible to have a good quality of life without a transplant?
Yes, it is possible to have a good life with lifelong transfusions and chelation therapy. However for a outcome a dedicated team of hematologist, pediatrician, endocrinologist, cardiologist and gastroenterologist is needed.
Why transplant if life is possible without it?
Getting transfusion for life will ensure a continued life; however a good quality of life requires a dedicated team and very intensive monitoring and chelation. This comes at an estimated lifelong cost of Rs 10 crore with the lifelong hassles of being a patient. However transplant offers the chance of cure so transplant is cost effective and best treatment for these children
Is Thalassemia preventable?
As we understand that Thalassemia is inherited, so every couple planning to have a child, they should get themselves tested to check if they have minor forms of Thalassemia. If both expecting parent have minor forms of Thalassemia then the chance of them having a child with a major form of Thalassemia is 25%. These parents should get the child tested in the 1st 20 weeks of pregnancy. If the child tested in mother’s womb is positive for Thalassemia they can opt for a voluntary abortion.
How is Thalassemia diagnosed?
It is diagnosed with the help of simple blood test known as Hemoglobin Electrophoresis or High performance liquid chromatography.

